The joint report covers data from 2023 and 2024 across 27 EU member states, the UK, and five additional countries. Three bacteria were the focus: Salmonella, Campylobacter, and carbapenemase-producing E. coli.
Campylobacter and the Ciprofloxacin Problem
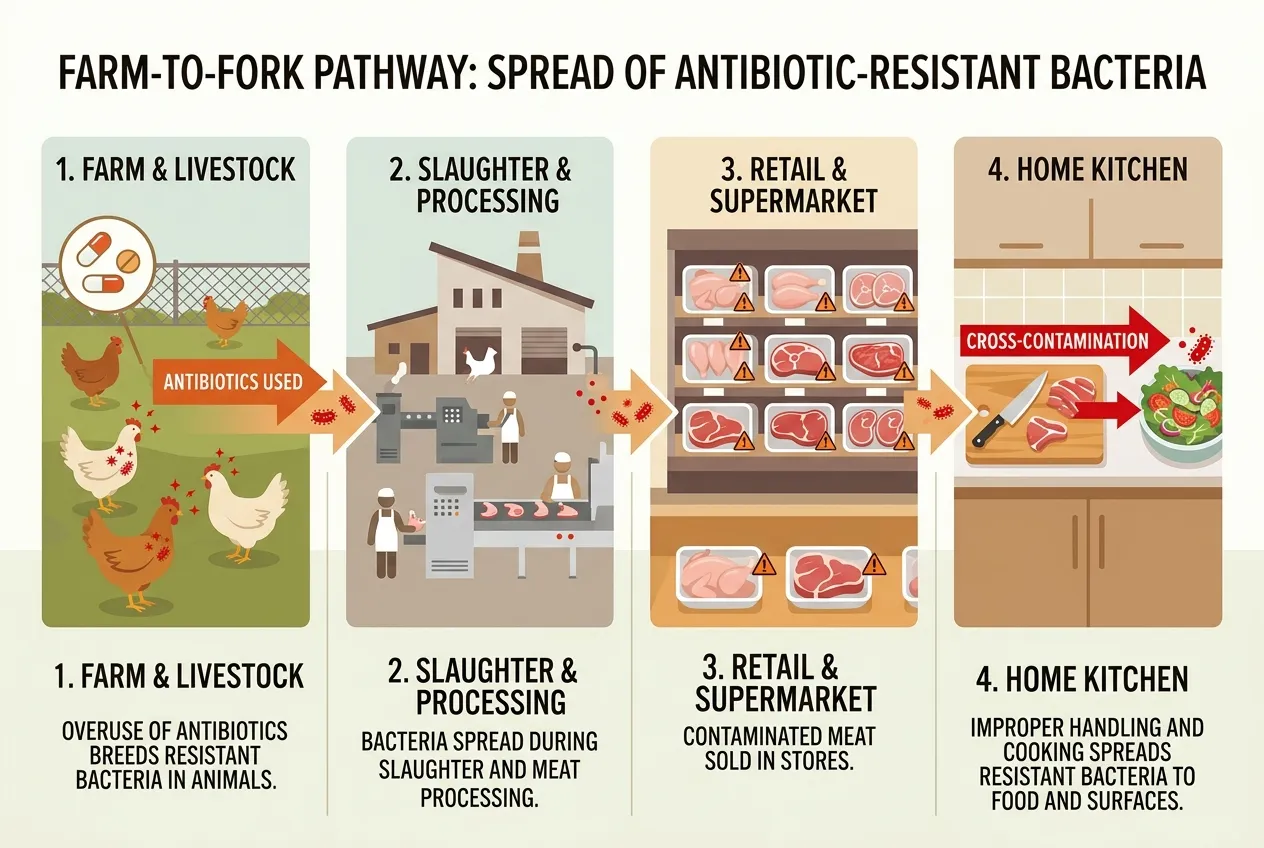
Campylobacter is the most commonly reported cause of bacterial foodborne illness in the EU. It is primarily transmitted through undercooked poultry. The 2026 report found widespread resistance to ciprofloxacin, a fluoroquinolone antibiotic that has historically been the first-line treatment for severe Campylobacter infections.
The finding is serious enough that EFSA now states ciprofloxacin is "no longer recommended for the treatment of human infections" with Campylobacter. That sentence marks a clinical shift driven by agricultural practice. A drug that doctors relied on has effectively been removed from the recommended toolkit for one of the most common foodborne pathogens, because resistance has become too widespread to make it reliable.
Resistance to ampicillin, tetracyclines, and sulfonamides was also described as persistently high in both Campylobacter and Salmonella.
Salmonella: Some Progress, Persistent Gaps
The Salmonella picture is more mixed. Ampicillin resistance declined in 19 countries over the past decade. Tetracycline resistance declined in 14 countries. Resistance in broilers and turkeys to these drugs showed downward trends, which EFSA attributes in part to tightened antibiotic stewardship policies.
But resistance to ciprofloxacin in Salmonella remains high across both human and animal sources. Improvement in some drugs has not extended across the board.
The Carbapenem Warning
The most significant concern in the 2026 report involves carbapenemase-producing E. coli. Carbapenems are described as "last-resort antimicrobials for humans." They are the drugs used when everything else has failed.
EFSA found carbapenemase-producing E. coli being detected in food-producing animals and meat across several countries, with detection numbers increasing. The report emphasizes that combined resistance to critically important antimicrobials remains "generally low." But the direction matters. The presence of carbapenem-resistant bacteria in the food supply is a signal that requires attention.