The Adventist Mortality Study (1958–1966)
The first formal research on this community began in the late 1950s. Researchers observed that Adventists had notably lower death rates from several major diseases compared to the general California population, particularly heart disease and certain cancers. This was striking enough to prompt more structured, long-term investigation.
Adventist Health Study 1 (AHS-1, 1976–1988)
The first full Adventist Health Study enrolled approximately 34,000 non-Hispanic White Adventists in California. Participants completed detailed diet questionnaires and were followed for over a decade.
The headline finding was stark: Adventist men lived an average of 7.3 years longer than other California men, and Adventist women lived 4.4 years longer than other California women. Vegetarian Adventist men in particular showed dramatically reduced risks of heart disease. Male vegetarians had a 37% lower risk of ischemic heart disease mortality than their non-vegetarian Adventist counterparts.
The study also linked frequent nut consumption (five or more times per week) to a roughly 31% reduction in lifetime heart disease risk, a finding that helped spark decades of subsequent research on nuts as a health food.
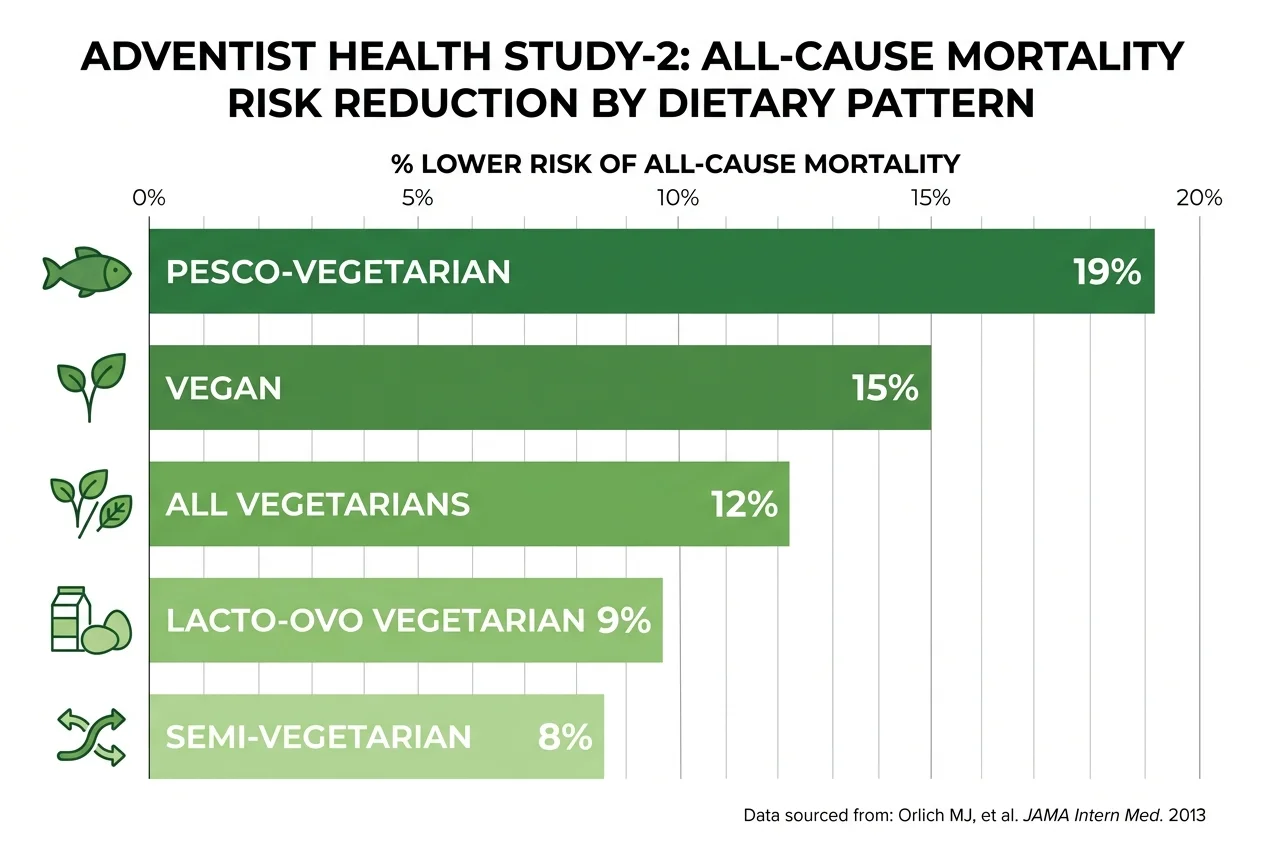
Adventist Health Study 2 (AHS-2, 2002–present)
AHS-2 is the most ambitious of the three studies, and the one that has generated the most influential published findings. Between 2002 and 2007, researchers enrolled 96,469 Seventh-day Adventists across the United States and Canada. Participants completed a detailed 50-page questionnaire covering diet, lifestyle, and health history, and have been followed with regular updates since.
A deliberate effort was made to recruit a racially diverse cohort. Approximately 27% of AHS-2 participants are Black, making it one of the few large-scale nutrition studies with meaningful representation across racial groups.
The analytic sample used in the primary mortality study comprised 73,308 participants, with 2,570 deaths recorded over a mean follow-up of 5.79 years.