Quick answer: Reheating rice is not enough if the Bacillus cereus toxin cereulide has already formed. The safety step is prevention: cool cooked rice quickly, refrigerate it promptly, and do not rely on a microwave to fix leftovers that sat out too long.
You cook a pot of rice, eat half, and leave the rest on the counter. You reheat it the next day. Seems harmless enough. People do this every day. But if those leftovers sat out long enough, reheating could actually make them more dangerous, not less.
The culprit is cereulide: a heat-stable toxin produced by the bacterium Bacillus cereus that no amount of cooking, microwaving, or boiling can destroy once it has formed. It's invisible, odourless, tasteless, and in rare but documented cases, deadly.
This is what food scientists call the "fried rice syndrome." It's more serious than most people realise, and understanding how cereulide forms is the only real protection against it.
What Is Cereulide? The Bacillus Cereus Toxin in Rice
Cereulide is a cyclic depsipeptide, a small ring-shaped molecule produced by certain strains of Bacillus cereus as a byproduct of bacterial growth. Unlike most bacterial toxins, cereulide is not a protein. That matters enormously, because it means:
- It survives temperatures up to 121°C (250°F), well above boiling point
- It is resistant to acidic and alkaline environments
- It cannot be broken down by the digestive enzymes in your gut
- No amount of reheating destroys it once it has been produced in food
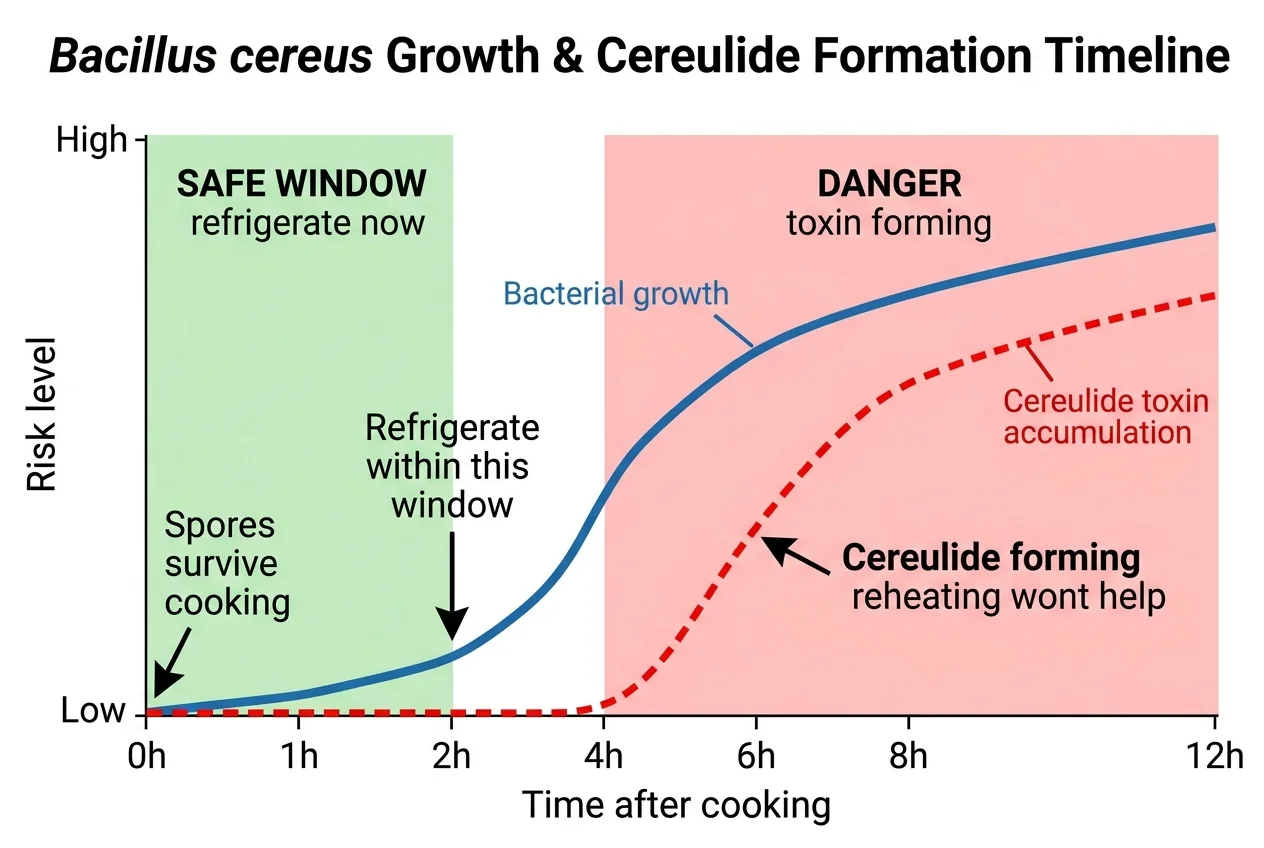
Bacillus cereus is a spore-forming bacterium that lives in soil and is commonly found on raw rice, grains, vegetables, and many other foods. The spores are extraordinarily robust: they survive normal cooking temperatures without difficulty. When cooked rice sits at room temperature, those spores germinate, bacteria multiply, and under the right conditions, primarily temperatures between 25°C and 30°C (77–86°F), toxin production begins.
The window is faster than most people expect. Significant cereulide accumulation can begin in as little as 6 hours at room temperature.
Why Reheating Rice Doesn't Destroy Cereulide
This is the most important thing to understand about cereulide: the bacteria and the toxin are separate problems, and cooking only addresses one of them.
Reheating rice to a safe internal temperature (165°F / 74°C, as the FDA recommends) will kill any live Bacillus cereus bacteria present. But if cereulide has already formed in the rice during the time it sat out, that toxin remains fully active in your food. You've killed the bacteria and left the poison.
Cereulide has been shown to survive autoclaving at 126°C for 90 minutes in laboratory conditions, far more heat than any home kitchen generates.
This is what separates cereulide from most foodborne hazards, where thorough cooking provides real protection. With cereulide, prevention must happen before the toxin forms, not after.
The Symptoms: Emetic vs. Diarrheal Illness
Bacillus cereus actually causes two distinct types of food poisoning, produced by two different toxins:
Emetic illness (cereulide):
- Caused by cereulide, which is preformed in food before it is eaten
- Symptoms: sudden, violent nausea and vomiting
- Onset: typically 30 minutes to 6 hours after eating
- Duration: usually resolves within 6–24 hours in healthy adults
- Most commonly associated with rice, pasta, and starchy foods
Diarrheal illness (enterotoxins):
- Caused by enterotoxins produced inside the body after ingesting live bacteria
- Symptoms: abdominal cramps and diarrhoea
- Onset: 6–15 hours after eating
- Most commonly associated with meat, poultry, soups, and sauces
Most cases of cereulide poisoning resolve without medical treatment. But the emetic form carries a serious risk in vulnerable populations, particularly infants, young children, and those with underlying liver conditions, where the toxin can cause devastating complications.
When It Turns Fatal
Cereulide is a mitochondrial toxin. It disrupts the electron transport chain, the process cells use to generate energy, which can trigger cell death in multiple organs simultaneously. In severe cases, this manifests as acute liver failure, rhabdomyolysis (muscle breakdown), metabolic acidosis, and multi-organ failure.
Documented fatal cases are rare but real. Research published in PMC has described cases of fulminant liver failure caused by cereulide, including a 20-year-old Belgian student who died after eating five-day-old pasta he had left at room temperature. In another documented case, a one-year-old child died of acute encephalopathy after consuming reheated fried rice.
A global analysis spanning 50 years identified 6,135 cases of B. cereus infection across 266 studies, with a mortality rate of approximately 0.05% among food poisoning cases. That's a small figure that still represents real deaths from what is widely considered a "minor" foodborne illness.
Children under two years old and school-age children appear disproportionately at risk for severe outcomes, including fulminant liver failure.
The 2026 Regulatory Wake-Up Call
In early 2026, cereulide moved firmly onto regulators' radar when Bacillus cereus toxin was detected in infant formula products from multiple manufacturers, triggering a precautionary global recall.
In response, the European Food Safety Authority (EFSA) published a rapid risk assessment establishing, for the first time, an Acute Reference Dose (ARfD) for cereulide in infants: 0.014 µg per kilogram of body weight. EFSA applied a standard uncertainty factor of 100, plus an additional factor of 3 to account for the reduced metabolic capacity of very young infants, reflecting how differently neonates process toxins compared to adults.
The assessment also established safety thresholds for reconstituted infant formula:
- Cereulide above 0.054 µg/L in standard infant formula may exceed the ARfD
- Cereulide above 0.1 µg/L in follow-on formula raises safety concerns
This regulatory milestone matters beyond infant formula: it signals that food safety authorities are beginning to quantify cereulide risk systematically, which may eventually lead to broader monitoring requirements across rice, pasta, and grain products.
The Right Prevention Strategy

Because cereulide cannot be destroyed by cooking, the only effective strategy is to prevent it from forming in the first place. That means controlling the window between cooking and refrigeration.
The 2-hour rule: Cool cooked rice (and other at-risk foods) to below 4°C within 2 hours of cooking. The FDA Food Code recommends this as the outer limit; many food safety specialists suggest aiming for 1 hour to be conservative.
How to cool rice quickly:
- Spread it thinly on a large baking tray or across two containers rather than leaving it in a deep pot
- Do not leave rice sitting on a warm hob or inside a warm covered pot
- For large batches, use an ice bath under the container
Storage and shelf life:
- Store in a shallow, airtight container in the refrigerator
- Consume refrigerated cooked rice within 2 days, not 3 or 4 days
- Do not reheat cooked rice more than once
Reheating — the limits: Reheating to 165°F/74°C all the way through will kill any bacteria present, reducing the bacterial load. But remember: if the rice sat out long enough for cereulide to form, reheating will not make it safe. When in doubt, discard it.
What This Means for Everyday Cooking
"Fried rice syndrome" sounds like a novelty food safety scare. In practice it points to a genuinely underappreciated hazard in the home kitchen. It strikes most during casual, low-attention cooking moments: the takeaway left on the counter, the pot of rice made hours before dinner, the office lunch left at room temperature.
The Cleveland Clinic's food safety guidance summarises it simply: cooked rice should be refrigerated within two hours and consumed within two days. These two rules eliminate virtually all real-world cereulide risk.
The complicating factor is that cereulide poisoning looks like ordinary food poisoning: nausea, vomiting, discomfort. Most people recover without ever knowing the cause. It's only in severe cases, particularly in children or people with liver conditions, that the full danger becomes apparent.
The Bottom Line
Cereulide is not a theoretical hazard. It's a real, heat-stable toxin that forms silently in cooked rice and other starchy foods when they sit too long at room temperature. It cannot be destroyed by cooking. Its only reliable countermeasure is time and temperature control: get cooked food into the refrigerator before the toxin has a chance to form.
The 2026 EFSA assessment of cereulide in infant formula is a signal that food authorities are taking this compound more seriously, and broader regulatory attention is likely to follow.
For most healthy adults, a case of cereulide poisoning means hours of misery. For infants, young children, and those with compromised liver function, it can mean something far worse.
IngrediCheck can't detect cereulide directly, since it forms after food is prepared rather than in the ingredients themselves. But IngrediCheck can help you understand the safety profile of packaged rice products, flag products under active recalls, and identify foods flagged for Bacillus cereus contamination, keeping you better informed about what's on your plate before you even start cooking.
If you want a faster reference for this specific hazard, keep the cereulide ingredient profile and the broader Ingredient Safety hub open alongside this guide.